Artery Occlusion
Retinal Arterial Occlusive Disease
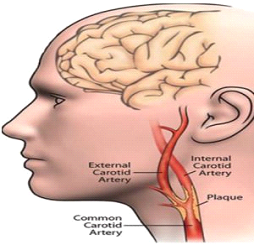
Deficient retinal artery circulation (Ischemia) may result from a disease process affecting anywhere between the carotid artery vessels of the neck to the tiny vessels in the retina. When this arises, this causes dead tissue (infarct) to develop due to lack of blood supply. Blood carries oxygen to the tissues. Our tissues of our bodies cannot survive without oxygen. When the retina is affected it leads to retina cell death and subsequent vision loss.
How do retinal artery occlusions happen?
Retinal artery occlusions occur when a blood clot, air bubble, piece of fatty deposit, or other object is carried in the bloodstream and lodges in a vessel and causes an embolism (obstruction of an artery). Emboli is the plural term.
The most common causes of emboli are high blood pressure, atherosclerosis (buildup of fatty plaque in the blood vessels) particularly in the carotid arteries, and high cholesterol. Rare causes of emboli include:
Risk factors for developing emboli:
Types of Retinal Artery Occlusion
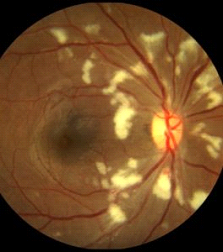
Capillary Retinal Arteriole Obstruction (Cotton-Wool Spots)
Sudden obstruction of the tiniest arteries (capillaries) around the optic nerve in the superficial layer of the retina causes infarct of the inner retina (cotton-wool spots). The effect on sight may include loss of vision or development of blind spots near/around your central vision. Diabetic retinopathy is the most common cause of cotton-wool spots. Many other diverse causes of cotton-wool spots have been identified and include:
Central Retinal Artery Occlusion (CRAO)
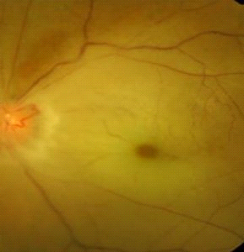
A central retinal artery occlusion occurs from a blockage of the main retinal artery as it enters the eye at the optic nerve. This causes sudden, complete, painless loss of vision in one eye. The retina becomes opaque and swollen, particularly in the macula, the center of the retina. With time, the central retinal artery reopens and the swelling clears; however, the effect on vision is usually permanent. Most cases of CRAO result in legal blindness.
The central retina artery travels through the optic nerve of the eye. CRAO is often caused by the presence of atherosclerosis at or just behind the optic nerve. As blood clots (thrombosis) form at or just behind the optic nerve where the central retinal artery passes through, it causes a CRAO.
Branch Retinal Artery Occlusion (BRAO)
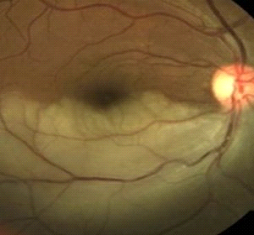
A branch retinal artery occlusion involves blockage of one or more of the smaller retinal arteries, a branch of the central retina artery. Symptoms may or may not exist depending on where the blockage develops. Blockage at any part of the smaller artery may arise from:
What are the symptoms?
Symptoms of a retinal artery occlusion vary based on the degree of impairment of blood flow to the eye. Sudden, painless loss of vision, either partial or complete, is the most common symptom. Loss of visual field, or a blurry or gray spot in the vision can also occur. If a blockage occurs away from the center of the retina no symptoms may develop, however, a permanent visual field loss develops that may be identified during your evaluation with the Ophthalmologist.
Diagnosis
During an eye exam, your ophthalmologist will dilate your pupil and look through a special lens at the inside of your eye. Often a clot or plaque can be seen inside the blocked artery. Your doctor may do fluorescein angiography to see what is happening with your retina. Yellow dye (called fluorescein) is injected into a vein, usually in your arm. The dye travels through the blood vessels. A special camera takes photos of the back of your eye as the dye travels throughout its blood vessels. This shows the extent of blood circulation and where there are deficiencies in flow.
Optical coherence tomography (OCT) is another way to look closely at the retina. A machine scans the retina and provides very detailed images of the retina and macula.
Your ophthalmologist will recommend that you see your primary care physician or cardiologist for a complete cardiovascular evaluation.
Treatment
Unfortunately, no specific ocular therapy has been found to be effective in improving the visual prognosis. Surgical intervention by way of the interventional radiologist or cardiologist has been attempted in the EAGLE trial. In that study blood clot dissolving medicine was injected into the ophthalmic artery to dissolve the embolus downstream. The results of that study were disappointing.
In very early cases, attempts can be made to lower the eye pressure with eye drops or a procedure called anterior chamber paracentesis. Pressure on the eye ball can also be tried. However, even with these attempts there is often little change in the blood flow status of the eye. In severe cases, abnormal blood vessels can grow that cause the eye pressure to rise and then pain to develop. In these cases, laser treatment can be used to help control the eye pressure and relieve pain.
Treatment consists of reducing the risks of new developments/injury from happening. Identifying the cause is very important as occlusive carotid disease is a main cause of retina artery occlusive disease. In my experience I have found undiscovered carotid artery stenosis (blockage) and heart arrythmias particularly atrial fibrillation as the main cause of central retinal artery occlusion. Your ophthalmologist will work with your PCP or Cardiologist’s office to schedule the indicated lab and imaging tests.
